
Antiviral drugs, such as oseltamivir (Tamiflu®) and zanamivir (Relenza®), bind neuraminidase, both interact with neuraminidase at sites crucial for its activity. In studying ways to prevent and battle influenza, research scientists have focused their efforts on blocking the actions of neuraminidase and hemagglutinin. Neuraminidase is an enzyme embedded in the virus membrane that facilitates newly synthesized viruses to be released from the host cells to spread the infection from one cell to another. Hemagglutinin aids the virus in fusing with host cells and emptying the virus’ contents inside. There are 18 types of hemagglutinin and 11 types of neuraminidase. The H#N# nomenclature for influenza A subtypes refers to the hemagglutinin (H) and neuraminidase (N) proteins that sit on the surface of the virus. Content Provider: CDC/ Douglas Jordan, Dr. The panel on the right identifies the virion’s surface protein constituents. This is a 3D illustration of a generic Influenza virion’s fine structure. The lag time between production in the spring and the flu season in the winter provides time for unexpected types to emerge. Each year, government agencies work with scientists to decide which strains to target in that year’s vaccine manufacturing. Scientific study is further complicated by the virus itself: there are 3 antigenic types of influenza virus that infect humans, (A, B, C), with various subtypes and strains. For instance, the virus can be transmitted among people not showing symptoms a n d cough, sneeze, or handshake can spread infectious droplets from someone who doesn’t know they’re sick. Scientists and policymakers face many challenges when studying the influenza virus. The diagram shows three Influenza viruses placed side by side, with eight color-coded RNA segments inside of each virus. The virus from the 2009 pandemic (right) has HA/NA proteins and RNA from Eurasian and North American swine instead of from humans like in previous years (left two viruses).Ĭontent Provider: CDC/Douglas Jordan, M.A. This diagram depicts how the human cases of swine-origin H3N2 Influenza virus resulted from the reassortment of two different Influenza viruses. The 2009 H1N1 virus is cited by some as a result of antigenic shift, because the virus was so different than previous H1N1 subtypes however, as there was no change in the actual hemagglutinin or neuraminidase proteins, it was technically a case of antigenic drift. The other source of change is “antigenic shift”, which results in a virus with a different type of hemagglutinin and/or neuraminidase, such as H3N2 to H1N1. With accumulating changes, these antibodies won’t work against the new changed virus, and the person can be infected again. If you get infected with a certain flu virus, or get a vaccine targeting a certain flu virus, your body develops antibodies to that virus. 
Every time the virus replicates, small genetic changes occur that result in non-identical but similar flu viruses: this is called “antigenic drift”. There are 2 ways a new influenza virus can emerge. Influenza A and B circulate each flu season, but it is the emergence of new influenza A strains that have been responsible for worldwide epidemics, or pandemics, in the past such as the 1918 ‘Spanish Flu’ pandemic and the 2009 H1N1 pandemic. However, the flu is responsible for millions of cases of severe illness and approximately 250,000 to 500,000 deaths worldwide each year. Responsible for more deaths than HIV/AIDS in the past century, the flu is one of the world’s’ most dangerous infectious diseases though it may not seem so, especially in the United States. 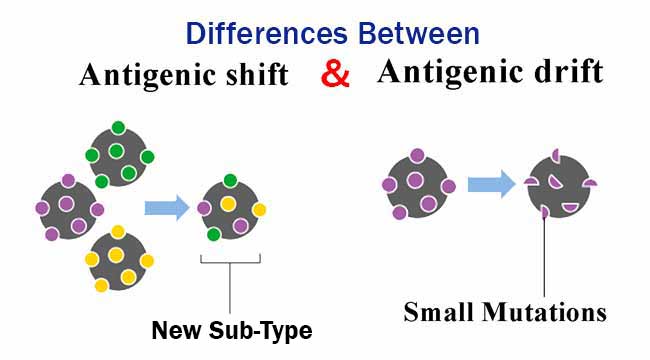
Influenza is a virus that straddles two worlds: that of the past and that of the future.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
